Fixation Base
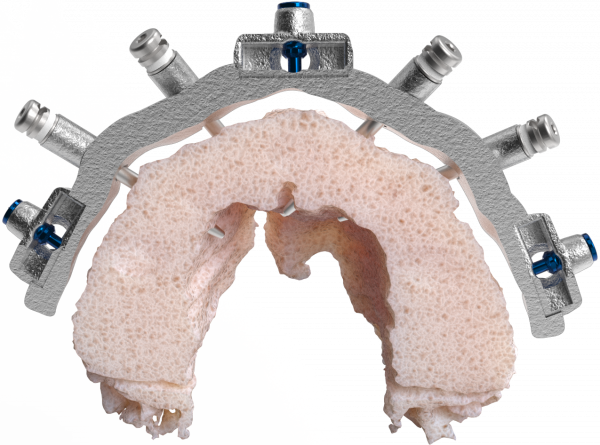
What is the Fixation Base?
- The Fixation Base is the second step of the CHROME GuidedSMILE process and sets the foundation for the surgery.
- All subsequent components clip into the CHROME Locs on the Fixation Base.
- It is unique in the industry because it is made of metal (CoCr) which means rigidity and stability.
- Our patented Fixation Base is designed using floating guide technology, meaning the guide does not contact bone, rather is supported by divergent pin placement.
- The Fixation Base’s initial function is bone reduction. The upper edge of the Fixation Base has been carefully created to indicate the level to which the bone needs to be reduced.
- The second function of the Fixation Base is to support the components: Osteotomy Guide, Carrier Guide, Provisional Prosthesis, and RAPID Appliance.
Download Your Free CHROME GuidedSMILE™
Ultimate Guide Now
What You'll Gain In This 90-Page Guide:
- Mastery of the 6-component & surgical protocol of the CHROME GuidedSMILE system
- Complete understanding of all necessary patient record requirements on a per-patient scenario
- Comprehensive day-of-surgery prosthesis conversation process
Available in digital or print format (free mailing included).
Frequently Asked Questions
Have question? We are here to help

No results found.
- Photographs: full face full smile photo, profile photo if Class II or III, and retracted photographs – front, left side, right side
- CBCT patient open biting on cotton rolls or the scanner bite stick. Place cotton rolls between cheeks and teeth.
- Maxillary & mandibular master casts or impressions. Must capture vestibule of the CHROME GuidedSMILE arch
- CO or CR bite registration
- Full GuidedSMILE CHROME Rx completed when uploading DICOM and photos
- Photographs: full face full smile photo, profile photo if Class II or III, and retracted photographs – front, left side, right side
- Master casts or impression of dentate arch (must capture vestibule), and impression of denture teeth and tissue
- Place 6 radiopaque markers on the denture (SureMark.com, or gutta percha 2mm round) – CBCT patient open biting on cotton rolls or the scanner bite stick.
- CO or CR bite registration
- Full GuidedSMILE CHROME Rx completed when uploading DICOM and photos
- Photographs: full face full smile photo, profile photo if Class II or III, and retracted photographs – front, left side, right side
- Master casts or impression of dentate arch and impression of denture teeth and tissue
- Place 6 radiopaque markers on the denture (SureMark.com, or gutta percha 2mm round) – CBCT patient closed, teeth together, not separated.
- CO or CR bite registration
- Full GuidedSMILE CHROME Rx completed when uploading DICOM and photos
- Photographs: full face full smile photo, profile photo if Class II or III, and retracted photographs – front, left side, right side
- Place 6 radiopaque markers on the denture (SureMark.com, or gutta percha 2mm round) – CBCT patient closed, teeth together, not separated.
- Bite should be worked out in the denture fabrication. If not, maximum opening of bite is 3mm.
- Full GuidedSMILE CHROME Rx completed when uploading DICOM and photos
Metal frames cause scatter and must be removed for the CBCT. If partial is needed for establishing bite, capture in an impression. If not, send master casts, opposing and bite.
The bite must be established through bite blocks and set‐ups. Once the case can be articulated then CHROME GuidedSMILE can move forward.
- 3mm is the maximum we will open in the laboratory w/o an open bite record being returned for verification. More than 3mm must be established clinically with CR bite, or through splint therapy. We can assist via our special JC Try‐In Repositioning Device.
- Tip: if distance between #9 & #24 gingival zeniths is less than 17mm (Shimbashi rule) then opening may be needed. Same if intervestibular is less than 35mm.
Seat using indicator and adjust until all the windows on the Pin Guide are in contact with the teeth. Caution, due to tooth undercut, not all of the window needs to be seated, just the occlusal/incisal. View how the Pin Guide seats on the model. This should be repeated intraorally.
If so, they may need to be manipulated into the Pin Guide similar to how they were impressed.
Modify the PG or extract teeth that do not impact the seating of the PG.
Refer to the notes! We make notes on extractions. Remove the specific teeth noted on the GSI form, due to mal-occlusion or draw.
if aggressive adjusting clearly changes the fit and seating accuracy of the PG, this may be cause enough to stop the surgery and capture new records to start over.
Flap the tissue until the Pin Guide seats. In other words, flap earlier on this arch. This is due to the initial impression not capturing the full vestibule, or the bone reduction is beyond the vestibule. Once seated, inspect and adjust if needed.
Must use manual clamping (fingers) to hold the Pin Guide and Fixation Base together. Pin Guide and Fixation base insertion accuracy is vital to the success of the case. The surgery could also be put on hold for a new Pin Guide to be ordered. The case should be returned to us to ensure accurate assembly.
Does it fit into the Fixation base passively? Do the CHROME Loc plungers easily and almost passively insert? If not, there could be material inside the CHROME Loc box preventing. This could also mean that someone heat cleaned the guide. Use a narrow bur and open the hold on the Pin Guide CHROME Loc loop until the plunger seats.
This probably means the model is not accurate, or perhaps the Pin Guide is fabricated with errors. The case must start with a fully seated Pin Guide. The case may have to be delayed. This is a clinical call based on how far off.
The pin can be re-seated. It will not function as the others. It will pull out every time, so please use care when pulling so as not to drop in the mouth. The plunger will still work.
Must use manual clamping (fingers) to hold the Pin Guide and Fixation Base together. Pin Guide and Fixation base insertion accuracy is vital to the success of the case. The surgery could also be put on hold for a new Pin Guide to be ordered. The case should be returned for us to ensure accurate assembly.
The protocol is to not flap first. Seat the Pin Guide, drill all the sites, remove the Pin Guide, flap and re-seat and insert pins. The flap can be made first. If so, carefully follow the instructions that are provided with each case. This is a ridge incision first, top of ridge flapped forward. Must use care with swelling from anesthesia. Must ensure the Pin Guide is very accurately seating even though there is no labial support.
Just like a denture, using indicator and finding the perfect seat. Be sure to account for swelling from inflammation from the anesthesia. Hold FIRM using two people or more, solid, consistent pressure. Do not use a surgical mallet until all the pins have been pushed in as far as they will go with finger pressure. Using a surgical mallet too early can put uneven pressure on the assembly of Pin Guide and Fixation Base.
This is critical. If the Pin Guide moves the teeth, the implants will be in the wrong position. Let us know early in the planning. We will fabricate a Pin Guide with opposing bite integrated. The patient will be closed biting on the Pin Guide while the facial pins are being seated. If there is no bite designed in the Pin Guide, use the palate for stability, or on lowers try to use the tissue.
If the Pin Guide is a replica of the denture, seat the Pin Guide and mark the nose and chin to verify final prosthetic accuracy. If this is a double arch, the Pin Guide will probably have a bite integrated, so the vertical is not centric and this technique cannot be used.
Options: 1) Complete upper full surgery and prosthetic conversion and then lower arch. The mandibular Pin Guide has a bite that is designed for the maxillary temporary prosthetic. In other words, when the max is finished, use the max teeth to ensure proper seating of the mandibular Pin Guide. 2) Seat both Pin Guides initially and drill all the max and man sites. Complete the max case, then flap the mandibular and the holes are already there for the pins. Both methods are acceptable. Follow the instructions included with each case for the flapping technique.
CHROME Loc’s are carefully checked. Guides may be going in crooked. Inspect the CHROME Loc Box for material. Might be clear, broken Pin Guide plastic that is hard to see. Perhaps the case was heat cleaned and warped. Carefully adjust the hold on the insertion part that is going in the box, until the plunger plunges.
Taper the end of the plunger tip, round off the edge.
Rongeurs twist and pull. Be delicate, full removal is not terrible, just inconvenient because it will not work as designed for the rest of the surgery.
NO Autoclave, only 20 minutes cold sterilization
The pin can be re-seated. It will not function as the others. It will pull out every time, so please use care when pulling so as not to drop in the mouth. The plunger will still work. Clinical chairside support may have extra plastic sleeves to replace the damaged one. CHROME is on the 3rd generation CHROME Loc design and a new design is being rolled out Q1 2019.
Exostosis that we missed. Lab may have trimmed the model and missed it. Inspect, a flap and adjust bone, or adjust metal with a disc, if possible – do not cut off a CHROME Loc or pin site.
Pin Guide may have seated crooked. This is BAD. If the teeth are still in, remove the Fixation Base and re-insert with the Pin Guide FULLY seated.
Mobile teeth may exist and the Pin Guide moved the teeth. If the Pin Guide has an integrated bite, re-start the case using the bite for seating the Pin Guide. Next time, inform the CHROME team of mobile teeth, especially of most or all are mobile. We will design a Pin Guide that seats against the opposing teeth.
Pin Guide is not seated correctly. Perhaps the bone is very soft and the malleting pushed the fixation base and oblonged the holes. This is bad. Suggest pulling the Fixation Base back out to mimic the GSI report images, pack gauze plugs between the Fixation base and the bone and be gentile during the surgery. Or, just use the Fixation Base for bone reduction and then freehand the implants using the Carrier Guide as just a guide for close implant location. These are just suggestions for a case that is not aligned correctly. This is not a surgical recommendation! These suggestions can lead to very unpredictable surgery and results.
Do not drill to depth. Drill ½ into the bone and use a surgical mallet to force the pins in. If it is too late and all the pins are in, this is bad. Suggest pulling the Fixation Base back out to mimic the GSI report images, pack gauze plugs between the Fixation base and the bone and be gentile during the surgery.
If you cannot back it out or easily remove, and you have an extra 2mm, leave it in place and use the other drill. Length can be measured by setting it next to a pin and using a sharpie. If this is the only drill, it must be removed. Remove the Pin Guide and the other pins and remove the drill. This is a last resort, as the removed pins will not fit the same as the initially did, and can be detrimental to the stability of the Fixation Base.
Remove and start over, or leave in if it is in the shaft of the Fixation Base
Be sure to have back-up pins and drills.
This is ok. Use the short pins and do not drill to full depth. Use a surgical mallet and tap the remaining 3-4 mm’s. If the plan calls for short pins and you only have long, a judgement call must be made. It may be okay to tap through the lingual cortical plate. This solution changes doctor by doctor and where the exit point is, mandibular or maxilla. Long Drills are 25mm and Short Drills are 21mm. Can leave the long drills protruding from the Fixation Base. This is the best option, as the trajectories of the pins should hold the base in place.
First question, do you remove? If it is not protruding through the Fixation hole then may just leave, especially if there are 3 more. If removal is needed, remove the Pin Guide, remove other pins and then Fixation base, and remove with rongeurs. Now what? Your drill broke. The drill is a 2.0mm that coordinates with the pin length, but, you can simply get another drill from another kit and use a sharpie to measure the length compared to the pin, and drill. You can always under drill and mallet into place.
Drill one at a time, push in the pin and move to the next site. Best practice is switch from far right or left, over to far opposite site. It is very important to not move the Fixation Base with the pin, rather, stop the pin at the Fixation Base sleeve.
‘Always mallet’ is a good protocol, even if it is just the last few millimeters. The pins should have resistance so that they do not come lose during the procedure. If the pin(s) is pushed to full depth easily, do not drill the next site to depth. Leave the drill a few mm’s short and mallet the pin until flush with the fixation base sleeve.
Very rare, but can use a drill or bur shank to hold the base in place.
Recommend back-up drills and pins kits
Don’t drill to depth. Stop 3-4mm or more short of the drill stop and mallet the pins in. If the Fixation base is lose after all the pins are seated then the bone is probably of very low density. There is no good solution, but can us a cotton plug and wedge between the bone and the Fixation Base to force the metal out, away from the bone. Try to mimic the image on the GSI report. There are images of how the metal should relate to the alveolar bone. Be very careful with assembling and disassembling the guides.
Check kit early to ensure passive fit. Spoons should fit with little to no resistance. If the spoons are a little lose, ensure the top of the Osteotomy guide sleeves and the spoon are flush seated when drilling all sites. Be sure if there are divergent, very close implants, that the spoons will seatfully w/o touching one of the other sites. This would have been checked in the lab, but a verification is still suggested.
Adjust as minimally as possible. Use a metal cutting bur and indicator in the guide tube to identify exactly where the contact it. Turn the Guide upside down and look up into the tube and visualization of the hang-up area should be evident. If the spoons are so lose that it appears the wrong design was made, clinical decision to move forward must be made. If the bone is very wide, proceeding may be ok.
Use the top of the spoon, make sure it is flat on the osteotomy guide and drill. If the ridge is very narrow use much more caution. Wrapping the spoon with Teflon tape is an option.
Assemble the spoon and drill and show the trajectory all the way to the bone. Often the sleeves seems lingual, but the sleeve is just the trajectory not the stopping point of the implants. In other words, the guide may look lingual, but it is in the position as designed.
Clinical judgement must be made if the guide clearly shows a wrong trajectory. Free-hand may be needed.
Clinical solution: see the drill touching the bone first.
Perhaps the bone was reduced too much. Bone level must be and extension of the Fixation Base and not angle up or down from that plane. If this is the case, use training on treating exposed threads. If anatomically and prostheticly allowable, place the implant deeper using a hand driver.
Do not use forceps. Do not want to dislodge the Fixation Base.
Call the rep. Call the company to find the rep. Call doctors in area with inventory! Find a compatible implant system and contact their rep. Try not to bail.
Bone reduction verification, MUA angle guide, delivery of the prosthetic and RAPID appliance, spacer for reflected soft tissue, verification that the driver is going in the right direction on angled implants (note the black square on angled sites – see instructions for specifics), tissue reflection.
This could mean any number of things went awry: Pin Guide was not seated correctly; angle implants are too deep or too shallow changing the connection position; implant chose a different path if they were inserted by hand, not guided; decide if they are placed in an area that is not acceptable – take an x-ray to verify that they are in an acceptable position and make a judgement to move or leave. The plan called for the implants to emerge in specific poition, and the fix is to modify the Carrier Guide and the prosthetic for pick-up. Be sure the Temp Cylinders do NOT contact the Carrier Guide or the prosthetic during the pick-up.
Verify that the implants are in the correct position. This can be observed visually through the carrier guide. If looks good, then the angled implants may be inserted in the wrong rotation. If it is, then the implant must be rotated, as little as just a few degrees. This should ‘right’ the MUA and Temp Cylinder. Also, verify that the abutment screw is in line with the black square on the Carrier Guide. This square is where the driver passes through to deliver the abutment screw, in the same trajectory as the implants. If the implant has been place with the correct indexing to the hex on the Osteotomy Guide, then the MUA may need to be remove and placed in one rotation clockwise or counterclockwise. Best course of action is to follow the implant guided kit to deliver the implant exactly as the Hex indicates.
YES. Must block out the pick-up material so as not to lock in the prosthetic. Can use light body, gloves for rubber damn, wax, other similar easily removed material.
NO, do not force or bend. It will break and be detrimental to success. Three main reasons it will not seat: 1) something is in the CHROME Loc box. Carefully inspect and clean 2) bone was not reduced sufficiently and is ‘holding it up’ 3) soft tissue is in the way. Make a stitch, or reflect more if needed.
1) Something is in the CHROME Loc box. Carefully inspect and clean
2) Bone was not reduced sufficiently and is ‘holding it up’
3) Soft tissue is in the way. Make a stitch, or reflect more if needed.
Yes, checking occlusion early is a good trick to know if there will be adjustment and to judge how surgery is going so far, to see that everything is stacking correctly.
If the CHROME Loc insert breaks there should be two remaining that work. That is sufficient. If more break, then hold down the Carrier Guide through the remaining procedures. If the guide broke in half, reinforce with acrylic on the INTAGLIO side, not the occlusal side. Do not want it raising the prosthetic. There is a gap under between it and the bone. This part can be reinforced.
This is very critical. The prosthetic must not be loaded if the torque does not meet the minimum number. We recommend using and ISQ device to check NCm’s. If you do not plan to load, at least pick up 3 of the Temp Cylinders on the MUA’s for tripoding. This is a good index for the delivery of the prosthetic in two to three months. The remaining implants can be picked up later. There is NOW WAY to do this once CHROME removed. Anything in the future is floating and cannot be picked-up. Pick up the RAPID appliance at this point as well if possible.
First check implant rotation on angled implants – best course of action is to rotate the implant until the Temp Cylinder is straight and parallel with the others. This means remove the MUA and use a hand driver to slightly adjust. Implant must be indexed precisely according to the Hex on the Osteotomy Guide for straight temp cylinders. Goal with CHROME is to deliver all parallel Temp Cylinders. This creates simple pick-up at surgery and ideal screw access in the final. If the Temp Cylinders are going to be picked up in the current tipped position, then adjust the prosthetic slightly to remove the contact. Sometimes the Temp Cylinders can be seated from the top down. In other words, seat the prosthetic on the remaining cylinders and deliver the crooked cylinder from the occlusal hole. If not, again, adjust the shaft of the prosthetic to accommodate. DO not over adjust, need 3mm from shaft to outside of prosthetic.
First check implant rotation on angled implants – best course of action is to rotate the implant until the Temp Cylinder is straight and parallel with the others. This means remove the MUA and use a hand driver to slightly adjust. Implant must be indexed precisely according to the Hex on the Osteotomy Guide for straight temp cylinders. Goal with CHROME is to deliver all parallel Temp Cylinders. This creates simple pick-up at surgery and ideal screw access in the final. If the Temp Cylinders are going to be picked up in the current tipped position, then adjust the prosthetic slightly to remove the contact. Sometimes the Temp Cylinders can be seated from the top down. In other words, seat the prosthetic on the remaining cylinders and deliver the crooked cylinder from the occlusal hole. If not, again, adjust the shaft of the prosthetic to accommodate. DO not over adjust, need 3mm from shaft to outside of prosthetic
Use #4 round bur and drill a hole through to the cylinder
Verify that the Carrier Guide is fully seated. If so, can shim a few millimeters and backfill. This will open the bite a little. If very high in the posterior, trim ½ of the pegs to remove resistance and shim half way to occlusion then adjust the occlusion.
Float the anterior and backfill. If double arch then trim the thicker of the two. Do not reduce to less than 8mm’s of vertical prosthetic material remaining. This very thin! MUST make an analog model with a flask as a back-up. MUST complete the RAPID pick-up to have a means of ordering another prosthetic during healing time. This could have been observed at the bone reduction time with the Carrier Guide and RAPID or Prosthetic seated for testing. This means it should not be a surprise.
Cut down the cylinders to be flush with the prosthetic.
Bite should have been verified at the RAPID and cylinders can be trimmed after the pick-up is completed. If the doctor wants to test the bite on the conversion prosthetic, then trim the cylinders in the mouth, or remove and trim. Mark with sharpie first. Trim with a 557 Carbide.
2019/2 $188
Quick-Up, adhesive blockout gaskets, syringeable blockout, applicators
YES – will not bond without the bonding agent
We only includes the SELF CURE ONLY Voco
Must be completely dry, including clean of blood. Future debonding eminent if the surface of the prosthetic cylinders is dry or contaminated.
Duralay, acrylic, Holmes Quick Set, GC Pattern Resin, Stellar. If these materials are not available find a doctor in the area and ask. Do not use standard acrylics.
Yes, very helpful, especially if not using VOCO or GC Pattern resin. If using acrylic or ERA pick-up (not advised materials), yes.
5mm distal from the posterior hole. Optional to grind down the posterior tooth down so that there is a flange extending posteriorly for the iJIG to capture the ridge when going to final. This is nice for capturing the posterior ridge in the future. This is up to the doctor if to leave the distal flange. If the doctor is going to make an iJIG then recommended to leave the flange. If picking up the RAPID (advisable), the posterior teeth are not removed and the ridge can be captured under the molars later.
Totally up to the doctor. But we’ve heard doctors add them for a total of 140 rule between all of them. We don’t recommend. Can add another implant in the area. Sleep implants and add to the RAPID, or iJIG later.
Ask the implant rep for a longer driver. Our clinical techs bring long lab drivers to surgeries.
Index the carrier where the hole is and adjust the prosthetic, making the hole smaller than the others so that not to jeopardize strength. Can also go back to the denture prosthetic and convert, All-on-4 style, as a last resort./p>
3, unless one is in the middle. Total clinician judgment call.
NO.
RAPID Appliance has two unique and very important primary functions. 1) Serves as a back-up indexed prosthetic in case the surgical prosthetic fails. Simply seat the RAPID, equilibrate, capture a bite and opposing and send to us for a new temporary, or final prosthetic. 2) Serves as the simplest method of transitioning to the final. Simply add tray adhesive to the intaglio, seat, equilibrate, capture a reline impression and send to us with bite opposing and photographs. The CHROME team can go to final or return what we call the Printed Try-In, a screw-down final prototype for clinical verification.
NO. If it is not picked up on the Carrier Guide while CHROME surgery is live, then the RAPID is not indexed to the implant, it’s just floating. This is not to be attempted. If the RAPID is not to be picked up at surgery, using lab analogs on the surgical prosthetic, make a stone model and use lab putty to flask over. This will allow the RAPID appliance to be placed in the flask, just like the conversion prosthetic, on temp cylinders on the analogs, and acrylic to be flowed in the flask to make the connection from RAPID to Temp Cylinder.
How can we help you today?
Can't find what you're looking for? No problem. Let us help.
ROE’s experts are dedicated to elevating your dental practice.
- Full-service national dental laboratory
- Comprehensive Certified Dental Laboratory (CDL) services
- Case planning support from 20+ Certified Dental Technicians
- Specialists in both fixed, removable, implant and full-arch dentistry
- Tailored support for all cases, from routine to complex
- National Association of Dental Laboratories (NADL) member
- Only FDA-approved materials used
- All products made in the USA
- Thousands of free online education materials




